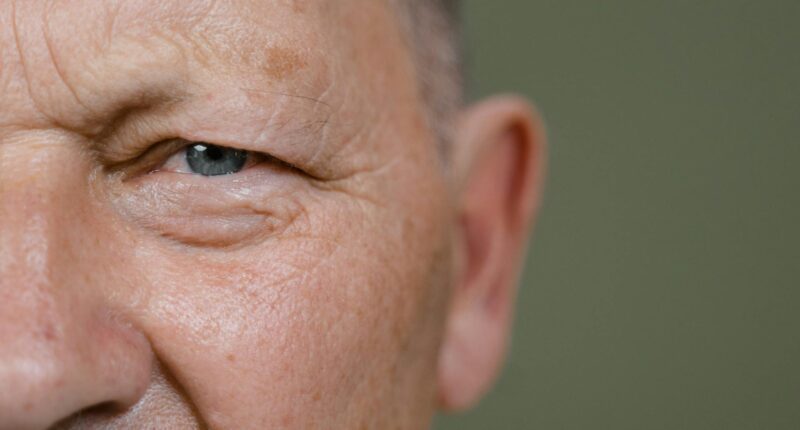
When battling cancer, the speed at which your face physically ages could be a critical indicator of your ultimate chances of survival.
According to new research published in the journal Nature Communications, an artificial intelligence tool developed by Mass General Brigham has proven that tracking “rapid facial ageing” over time is a highly accurate, non-invasive predictor of cancer mortality.
By analysing simple photographs, the deep-learning algorithm can estimate a patient’s biological age, revealing hidden prognostic signals that traditional chronological age cannot capture.
The speed of biological ageing
The researchers analysed two photographs from 2,276 patients with varying types of cancer who received radiation therapy at Brigham and Women’s Hospital between 2012 and 2023.
They calculated two crucial metrics:
- FaceAge Deviation (FAD): How biologically old or young a patient looks relative to their actual chronological age in a single baseline photo.
- Face Ageing Rate (FAR): The change in the AI’s age estimate between two photos, divided by the time interval between them.
The study revealed that the facial ageing of cancer patients vastly outpaced their chronological ageing by a median of 40 per cent. Crucially, the researchers found that a higher FAR — representing accelerated biological ageing between treatments — was significantly associated with a decreased probability of survival. This predictive effect was most robust when the interval between the two photographs was two years or more.
A non-invasive prognostic biomarker
“Deriving a Face Ageing Rate from multiple, routine facial photographs allows for near real-time tracking of an individual’s health,” explained Dr Raymond Mak, a radiation oncologist at the Mass General Brigham Cancer Institute and co-senior author of the study. “Our study suggests that measuring FaceAge over time may refine personalised treatment planning, improve patient counselling, and help guide the frequency and intensity of follow-up in oncology.”
When patients exhibited both a high FAD (looking significantly older than their actual age at baseline) and a high FAR (rapidly ageing between scans), their survival probabilities were the poorest. However, the researchers noted that the dynamic FAR measurement was a much more stable predictor of long-term survival outcomes than a single FAD reading.
Dr Hugo Aerts, director of the Artificial Intelligence in Medicine programme at Mass General Brigham, noted that extracting this data from simple, routine photographs offers an incredibly cost-effective, non-invasive biomarker.
The public can currently test the baseline AI tool themselves by submitting a photograph to the research team’s newly launched institutional web portal.